Plans To Recall Some Over The Counter Meds
Health chiefs are saying over-the-counter household medications such as Sudafed, Nurofen, and Day & Night Nurse could be banned from shelves because of their links to extremely rare brain disorders.
Sudafed, Nurofen and Day & Night Nurse could be banned health report states | Metro News
What is Pseudoephedrine:
Pseudoephedrine is a popular over-the-counter medication used to relieve nasal congestion caused by allergies, colds, and other respiratory illnesses. It belongs to a class of drugs known as decongestants and is sold under various brand names, including Sudafed, Sudafed PE, and Afrinol. Pseudoephedrine works by narrowing the blood vessels in the nasal passages, reducing inflammation and congestion.
Pseudoephedrine was first approved by the US Food and Drug Administration (FDA) in 1950 and has been available for use in the United States since then. It is commonly found in combination with other medications, such as antihistamines, in over-the-counter cold and allergy remedies.
While pseudoephedrine is generally considered safe when used as directed, it can have side effects, including increased heart rate, elevated blood pressure, nervousness, restlessness, and difficulty sleeping. These side effects are typically mild and short-lived, but in rare cases, they can be more severe.
One of the major concerns with pseudoephedrine is its potential for abuse. Pseudoephedrine can be used to make methamphetamine, a highly addictive drug. As a result, in 2005, the US government passed the Combat Methamphetamine Epidemic Act, which placed restrictions on the sale of pseudoephedrine-containing products.
Under this law, consumers must show a photo identification and sign a logbook to purchase products containing pseudoephedrine. They are also limited in the amount they can purchase in a given time period. These measures have been effective in reducing the number of clandestine methamphetamine labs in the United States.
Despite these restrictions, some individuals still attempt to obtain pseudoephedrine illegally, often by purchasing it in large quantities from multiple retailers or through online sources. This has led to ongoing concerns about the abuse potential of pseudoephedrine and the need for continued monitoring and regulation.
Overall, while pseudoephedrine can be an effective treatment for nasal congestion, it is important to use it only as directed and to be aware of its potential side effects and abuse potential. If you have any questions or concerns about using pseudoephedrine or other medications, it is always best to consult with a healthcare professional.
Posterior Reversible Encephalopathy syndrome (PRES):
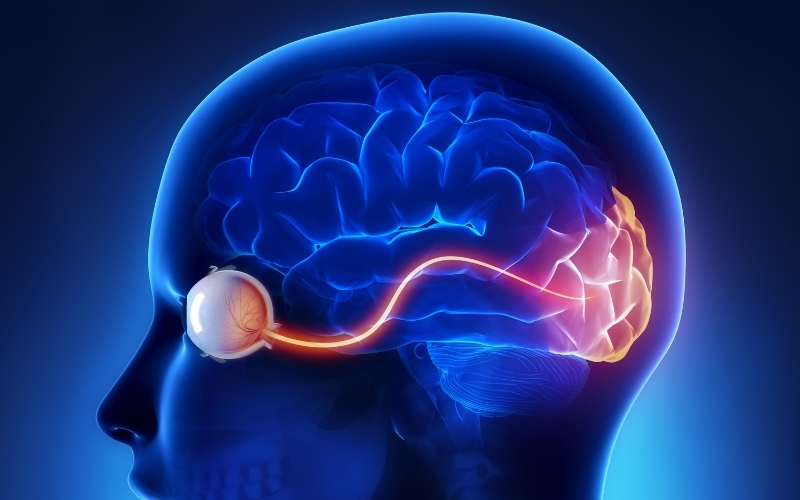
Posterior Reversible Encephalopathy Syndrome (PRES) is a rare and potentially life-threatening neurological disorder that is characterized by changes in the brain that can lead to a range of symptoms, including seizures, headaches, and visual disturbances. PRES typically occurs in individuals who have an underlying medical condition or who have experienced a traumatic event, such as a stroke or a severe injury.
Symptoms of PRES can develop rapidly and may include headaches, confusion, seizures, and vision changes. In some cases, the symptoms may progress to more serious complications, such as cerebral edema (swelling of the brain) or intracranial hemorrhage (bleeding in the brain). If left untreated, PRES can lead to long-term neurological damage or even death.
The exact cause of PRES is not fully understood, but it is believed to be related to changes in the blood vessels of the brain. These changes may be triggered by a variety of factors, including high blood pressure, immunosuppressive medications, infections, or autoimmune disorders. In some cases, PRES may occur following a traumatic event, such as a stroke or a severe head injury.
Diagnosis of PRES typically involves a combination of physical exams, imaging tests, and neurological assessments. A brain MRI is often used to identify the characteristic changes in the brain that are associated with PRES. Additional tests, such as blood tests or lumbar puncture (spinal tap), may be used to rule out other possible causes of the symptoms.
Treatment of PRES typically involves addressing the underlying medical condition or trigger that caused the symptoms. For example, if high blood pressure is identified as the cause, medications may be prescribed to lower blood pressure. In some cases, medications such as anticonvulsants or steroids may be used to help manage the symptoms of PRES.
The prognosis for individuals with PRES varies depending on the severity of the symptoms and the underlying cause of the condition. In many cases, individuals will experience a full recovery with prompt and appropriate treatment. However, some individuals may experience long-term neurological damage or other complications.
To prevent PRES, it is important to maintain good overall health and to manage any underlying medical conditions that may increase the risk of developing the disorder. This may involve making lifestyle changes such as improving diet and exercise habits, managing stress levels, and monitoring blood pressure and other vital signs.
Posterior Reversible Encephalopathy Syndrome is a rare but potentially life-threatening neurological disorder that requires prompt diagnosis and treatment. Individuals who experience symptoms of PRES, such as headaches, seizures, or vision changes, should seek medical attention right away to prevent serious complications. With appropriate treatment and management, many individuals with PRES can experience a full recovery and regain their quality of life.
Reversible Cerebral Vasoconstriction Syndrome (RCVS)’:
Reversible Cerebral Vasoconstriction Syndrome (RCVS) is a rare but potentially serious condition that affects the blood vessels of the brain. The syndrome is characterized by recurrent, severe headaches that are often accompanied by other neurological symptoms such as visual disturbances, seizures, and confusion. RCVS is caused by a temporary narrowing of the blood vessels in the brain, which can result in reduced blood flow and damage to brain tissue. Fortunately, RCVS is usually reversible and can be managed with appropriate treatment.
Causes of RCVS:
The exact cause of RCVS is not well understood, but it is believed to be related to the sudden and intense constriction (narrowing) of the blood vessels in the brain. This constriction can be triggered by a number of factors, including:
- Medications: RCVS can be a side effect of certain medications, such as selective serotonin reuptake inhibitors (SSRIs), ergotamines, and triptans.
- Illicit drugs: The use of illicit drugs such as cocaine or amphetamines can also trigger RCVS.
- Hormonal changes: Hormonal changes, such as those that occur during pregnancy or menopause, have been associated with RCVS.
- Physical exertion: RCVS has been reported in individuals who have engaged in strenuous physical activity or weightlifting.
Symptoms of RCVS:
The symptoms of RCVS can vary in severity and duration. Some people may experience only mild symptoms, while others may experience severe headaches and other neurological symptoms. The most common symptoms of RCVS include:
- Sudden and severe headache
- Visual disturbances, such as blurry vision or double vision
- Seizures
- Confusion or disorientation
- Nausea or vomiting
- Neck stiffness or pain
Diagnosis of RCVS:
Diagnosing RCVS can be challenging because the symptoms are similar to those of other neurological conditions, such as migraines or strokes. If RCVS is suspected, the healthcare provider may order a number of tests to confirm the diagnosis, including:
- Brain imaging: Magnetic resonance imaging (MRI) or computed tomography (CT) scans may be used to visualize the blood vessels in the brain and identify any areas of constriction.
- Cerebral angiography: This test involves injecting a contrast dye into the blood vessels of the brain and using X-rays to create detailed images of the blood vessels.
- Lumbar puncture: A sample of cerebrospinal fluid (the fluid that surrounds the brain and spinal cord) may be taken and analyzed to rule out other conditions.
Treatment of RCVS:
Treatment for RCVS typically involves managing the symptoms and addressing any underlying causes. Medications such as calcium channel blockers and anti-epileptic drugs may be used to help prevent constriction of the blood vessels and manage seizures. In severe cases, hospitalization may be necessary for close monitoring and management of symptoms.
Most people with RCVS recover completely within a few weeks to months, although some may experience recurrent episodes. It is important to follow up with a healthcare provider regularly to monitor for any long-term complications and to manage any underlying conditions that may have triggered the RCVS.
Reversible Cerebral Vasoconstriction Syndrome is a rare but potentially serious condition that affects the blood vessels of the brain. It can be triggered by a number of factors, including medications, illicit drugs, hormonal changes, and physical exertion. Early diagnosis and treatment are important to prevent complications and ensure a full recovery. If you experience any of the symptoms associated with RCVS, it is important to seek medical attention immediately.
iSchaemia:
iSchaemia, also known as ischemia, is a medical condition characterized by a restriction in blood supply to an organ or tissue. This can occur in any part of the body, including the heart, brain, limbs, and internal organs. iSchaemia is a serious condition that can cause tissue damage or death if left untreated.
The most common cause of iSchaemia is a blockage in the blood vessels that supply the affected organ or tissue. This can be caused by a variety of factors, including blood clots, plaque buildup in the arteries, or compression of blood vessels due to injury or other medical conditions. In some cases, iSchaemia can also be caused by a decrease in blood flow due to low blood pressure, shock, or other circulatory problems.
The symptoms of iSchaemia depend on the location of the affected organ or tissue. In the case of iSchaemic heart disease, for example, patients may experience chest pain, shortness of breath, and fatigue. iSchaemia of the brain can cause symptoms such as confusion, dizziness, and difficulty speaking or moving. iSchaemia of the limbs can cause pain, numbness, and weakness.
Diagnosis of iSchaemia typically involves a physical exam, medical history review, and diagnostic tests such as imaging studies, blood tests, and electrocardiograms (ECGs). Treatment for iSchaemia depends on the underlying cause and the severity of the condition. In some cases, medications such as blood thinners or antiplatelet drugs may be used to prevent further blood clots from forming. Surgery or other invasive procedures may also be necessary to restore blood flow to the affected area.
Prevention of iSchaemia involves a healthy lifestyle and management of underlying medical conditions such as high blood pressure, high cholesterol, and diabetes. Quitting smoking, exercising regularly, and maintaining a healthy weight can also help reduce the risk of iSchaemia.
iSchaemia is a serious medical condition that can cause tissue damage or death if left untreated. It can affect any part of the body and is typically caused by a blockage or restriction in blood flow. Diagnosis and treatment of iSchaemia involve a thorough evaluation by a medical professional, as well as management of underlying medical conditions and lifestyle changes to reduce the risk of recurrence.
Conclusion
PRES and RCVS can involve reduced blood supply (ischaemia) to the brain and may cause major and life-threatening complications in some cases.
Signs of PRES often include headaches, vision problems, mental changes, seizures, and swelling in the brain, according to the NHS.
Pseudoephedrine is already known to pose a slight risk to the heart including strokes and heart attacks.
Other decongestants, such as products made by Benylin, Nurofen, and Day & Night Nurse, would also be affected if any change was necessary.
Dozens of own-brand remedies — including ones at Boots and Lloyds — also contain the chemical.
The decongestant works by narrowing swollen blood vessels in the sinuses — which causes the nose to become blocked in the first place.
The Medicines and Healthcare Products Regulatory Agency (MHRA), which polices the safety of drugs used in Britain, is behind the review.
The European Medicines Agency (EMA) launched its own review into the safety of medicine less than a fortnight ago.
#productrecall #ema #mhra #fda #decongestants #pseudoephedrine #pres #rcvs #ischaemia #sudafed #nurofen #daynurse #nightnurse