Cosmetic Hygiene in Retail: Why Sealed Products Are Not a Luxury but a Necessity
Cosmetic hygiene in retail: Why unsealed beauty products pose serious health risks, including eye infections, and why stricter safety measures are needed.
DISABLED ENTREPRENEUR – DISABILITY UK
Disability UK Online Health Journal – All In One Business In A Box – Forum – Business Directory – Useful Resources – Health – Human Rights – Politics
DISABLED ENTREPRENEUR – DISABILITY UK
Disability UK Online Health Journal – All In One Business In A Box – Forum – Business Directory – Useful Resources – Health – Human Rights – Politics
Browsing Category

Cosmetic hygiene in retail: Why unsealed beauty products pose serious health risks, including eye infections, and why stricter safety measures are needed.
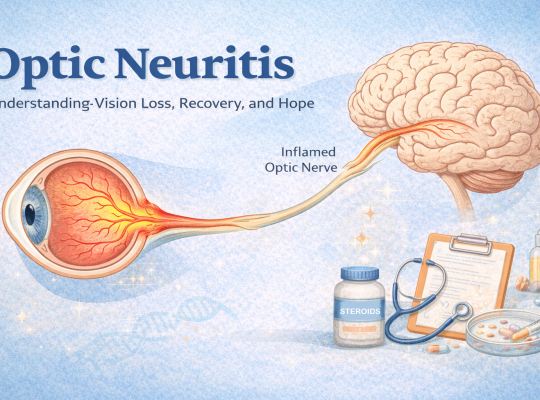
Optic neuritis explained: symptoms, treatment, recovery, and hope. Learn how to support someone with vision loss and explore future treatments like bionic eyes.

Cataracts and intraocular lens (IOL) implants can affect people of any age, including after head trauma or autoimmune conditions. Learn about symptoms, lens movement, worst-case scenarios, and future vision technologies such as bionic lenses and artificial eyes.

When most people hear the word cataracts, they picture someone in their 70s or 80s. I used to think the same, but at just 15 years old, I was diagnosed with cataracts in both eyes after noticing trouble with my vision. A year later, at 16, I underwent cataract removal surgery in my right eye.
Comprehensive guide to cataracts, symptoms, diagnosis, surgery risks, PCO, driving safety and whether cataracts may support a PIP claim in the UK.

Choosing a cosmetic eye care specialist is a personal decision that deserves time and thoughtful consideration. This isn’t just about appearances; it’s about placing trust in someone who will work near one of the most sensitive and expressive parts of the body.

Regarding modern insurance scoring, tiny details become data points, and patterns become conclusions. Once you measure, record, and fact-base your rate, minor details behind the wheel become significant. Making deliberate decisions frequently enables one to avoid accusations of recklessness or caution without uttering a single word.

Cataracts, a common eye condition characterized by clouding of the lens, often lead to blurred vision and, if left untreated, can result in significant vision impairment. While cataracts are frequently associated with aging, emerging evidence suggests a potential link between cataracts and autoimmune diseases, particularly Multiple Sclerosis (MS).
Public awareness, stricter regulations, and the promotion of low-noise fireworks and drone shows are crucial steps toward more inclusive and considerate celebrations.
The Spoon Theory offers a simple yet profound framework for understanding the complexities of living with MS and other chronic illnesses. It illustrates how daily activities can feel like constant, exhausting choices that most people take for granted. For those with MS, managing spoons is an ongoing process requiring patience, understanding, and often, self-compassion.