Empty Nest Syndrome: When Silence Feels Loudest
A compassionate guide to Empty Nest Syndrome, exploring its emotional impact and offering practical ways to cope with loneliness, especially for parents without partners or family support.
DISABLED ENTREPRENEUR – DISABILITY UK
Disability UK Online Health Journal – All In One Business In A Box – Forum – Business Directory – Useful Resources – Health – Human Rights – Politics
DISABLED ENTREPRENEUR – DISABILITY UK
Disability UK Online Health Journal – All In One Business In A Box – Forum – Business Directory – Useful Resources – Health – Human Rights – Politics
Browsing Category
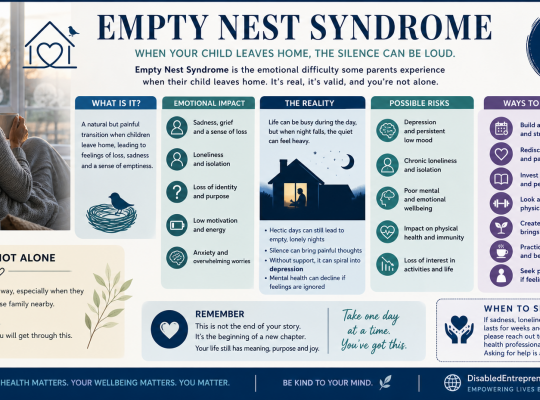
A compassionate guide to Empty Nest Syndrome, exploring its emotional impact and offering practical ways to cope with loneliness, especially for parents without partners or family support.

An in-depth look at depression, trauma, and PIP assessments, exploring why outward behaviour does not reflect mental health and how self-help strategies support recovery.

How insensitive questioning in healthcare can trigger intrusive thoughts and trauma responses. Learn about the psychology behind trigger wording, patient rights, and legal protections in the UK.

Exploring psychology, human behaviour, and why healthcare professionals should avoid trigger wording when discussing mental health with patients. Learn about patient rights and UK legal protections.

Encouraging disabled and long-term unemployed people to learn new skills or start a business can improve financial independence, mental health, and create a more sustainable future for generations to come.

Young adult detachment issues and separation guilt affect both generations. Explore how empty nest syndrome and young adults’ guilt intersect, and how families can navigate independence with empathy.

What depression really feels like when money runs out: the hidden impact of sanctions, unemployment, and trauma, plus practical steps to help people slowly rebuild hope.

Celebrity culture has long been a source of fascination for the public, offering a glimpse into the glamorous lives of actors, musicians, and influencers. However, behind the glitz and glamour, there is often a darker side that can lead to severe mental health challenges, including depression and substance abuse.

An honest, first-person article on relationship breakups, unrequited love, divorce, and healing, offering practical guidance on what to do and what not to do when your heart is broken.

OCD is a powerful and often debilitating condition, but it is rooted in the mind’s fundamental desire to protect the individual from harm. By understanding and addressing the fears that drive OCD, sufferers can begin to reclaim their lives from the grips of anxiety and compulsive behaviors.