Empty Nest Syndrome: When Silence Feels Loudest
A compassionate guide to Empty Nest Syndrome, exploring its emotional impact and offering practical ways to cope with loneliness, especially for parents without partners or family support.
DISABLED ENTREPRENEUR – DISABILITY UK
Disability UK Online Health Journal – All In One Business In A Box – Forum – Business Directory – Useful Resources – Health – Human Rights – Politics
DISABLED ENTREPRENEUR – DISABILITY UK
Disability UK Online Health Journal – All In One Business In A Box – Forum – Business Directory – Useful Resources – Health – Human Rights – Politics
Browsing Category
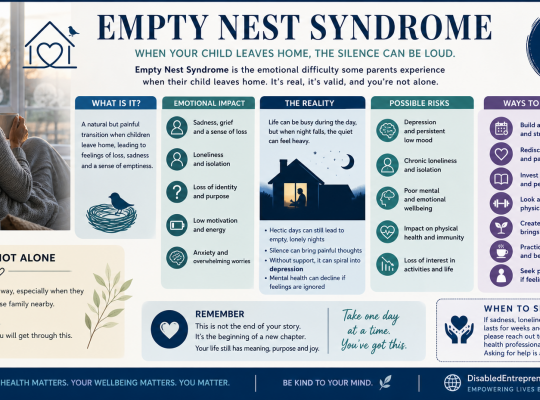
A compassionate guide to Empty Nest Syndrome, exploring its emotional impact and offering practical ways to cope with loneliness, especially for parents without partners or family support.

University students often experience anxiety while waiting for results, especially those with mental health conditions. Learn why it happens and practical ways to manage intrusive thoughts.

An in-depth look at depression, trauma, and PIP assessments, exploring why outward behaviour does not reflect mental health and how self-help strategies support recovery.

Working and studying with anxiety can be overwhelming. Learn about challenges, reasonable adjustments, communication needs, and practical coping strategies.

While exercise has evident benefits, it’s crucial to understand its role within the broader context of depression treatment. Exercise alone is not a standalone cure for depression but can be a highly effective complementary treatment. For some individuals with mild to moderate depression, regular physical activity might be sufficient to manage their symptoms. However, those with severe depression typically require a combination of treatments, including medication, psychotherapy, and lifestyle changes.

Young adult detachment issues and separation guilt affect both generations. Explore how empty nest syndrome and young adults’ guilt intersect, and how families can navigate independence with empathy.

A recent study by the Resolution Foundation has revealed a concerning trend in England and Wales: 1.2 million children are now living with a disability, with the most significant increase observed among teenagers. This statistic is a sobering reminder of the growing challenges facing today’s youth, particularly regarding mental health issues, which have seen a sharp rise in recent years.

Achieving a balanced life requires more than just managing time—it involves creating spaces that support your physical and mental needs. Ergonomics bridges this gap, offering practical solutions to ease daily stressors and enhance overall well-being.

Student finance in the UK is designed to support students with the costs of higher education. This includes tuition fee loans, maintenance loans, and grants. While these resources are invaluable, the process of applying for them can be daunting, especially for disabled students and those facing unique circumstances.

Autoimmune disorders can significantly impact an individual’s ability to work, posing challenges related to health, safety, and employer liability. Understanding the limitations faced by individuals with autoimmune diseases in the workplace is crucial for ensuring their well-being and addressing the concerns of employers.