My Story and what happened when my eyesight changed far too soon, and the essential facts everyone should know.
When most people hear the word cataracts, they picture someone in their 70s or 80s. I used to think the same, but at just 15 years old, I was diagnosed with cataracts in both eyes after noticing trouble with my vision. A year later, at 16, I underwent cataract removal surgery in my right eye.
I’m sharing this to raise awareness: cataracts can affect young people too.
Let’s break down what cataracts are, how they develop, who is at risk, and what to watch out for. Then I’ll talk about something many people don’t know about: secondary cataracts, also called Posterior Capsule Opacification (PCO), which I was recently diagnosed with in my operated eye.
What is a Cataract?
A cataract is a clouding of the eye’s natural lens; the lens sits behind the iris (The coloured part of your eye) and focuses light onto the retina so you can see clearly. When the lens becomes cloudy, light can’t pass through properly; vision becomes blurred, hazy, or dim, almost like looking through a foggy window.
Cataracts are extremely common and are one of the leading causes of vision impairment worldwide.
How Do Cataracts Develop?
The lens of the eye is made mostly of water and proteins. As we age, or under certain conditions, these proteins can begin to break down and clump together. This clumping creates a cloudy area in the lens.
Cataracts can develop:
- Slowly over many years
- Rapidly, in some cases (especially in younger individuals)
- In one or both eyes
Types of Cataracts:
- Nuclear Cataracts: form in the centre of the lens
- Cortical Cataracts: start at the edges and move inward
- Posterior Subcapsular Cataracts: form at the back of the lens and often affect vision more quickly
There are also fewer common types of cataracts that can affect younger people, including:
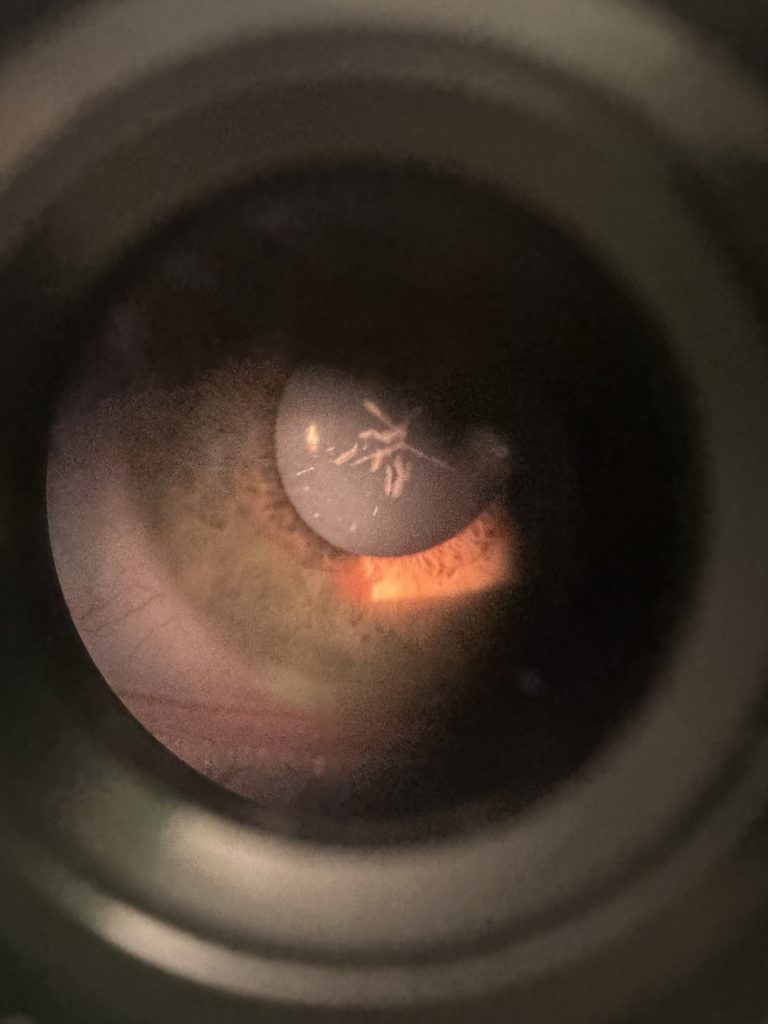
My Actual Snowflake Cataract
Snowflake Cataracts: a distinct type of cataracts often associated with diabetes and typically seen in younger individuals, they appear as white snowflake-like opacities in the lens and can progress quickly.
In my case, I was diagnosed with a snowflake cataract, something most people don’t even realise can happen to teenagers.
Signs and Symptoms of Cataracts
Common symptoms include:
- Blurry or cloudy vision
- A hazy or foggy view
- Increased sensitivity to light
- Halos around lights
- Difficulty seeing at night
- Faded or yellowed colours
- Frequent changes in glasses prescription
For me, the changes were subtle at first; my vision just didn’t feel right, but over the coming months, my vision rapidly declined, and the cloudiness became more noticeable.
Who is Most at Risk?
Higher risk groups include:
- Adults over 60
- People with diabetes
- Those with a family history of cataracts
- People who have had eye injuries
- Long-term steroid users
- Smokers
- People with high UV exposure
- Children and teenagers (congenital or developmental cataracts)
Yes – teenagers.
Being 15 and being told I had cataracts in both eyes felt surreal; I didn’t fit the stereotype, but cataracts don’t follow stereotypes.
What is a Secondary Cataract?
Here’s something many people don’t know: cataracts can’t technically “grow back” once removed. However, you can develop something called a secondary cataract, medically known as:
Posterior Capsule Opacification (PCO)
This is not a new cataract; it’s a clouding of the membrane (capsule) that holds the artificial lens in place after surgery.
How do secondary cataracts develop?
During cataract surgery, the cloudy natural lens is removed, but the thin capsule that surrounds it is left in place to support the artificial lens implant.
Over time, leftover lens cells can grow and multiply on the back of that capsule. This causes it to become cloudy, similar to how the original cataract affected vision.
This cloudiness can develop:
- Weeks after surgery
- Months later
- Or even years later
In my case, it developed exactly 10 years after my original surgery.
Who is Most at Risk for Secondary Cataracts?
PCO is actually quite common; studies suggest that a significant percentage of people who undergo cataract surgery will develop some degree of Posterior Capsule Opacification.
Risk factors include:
- Younger age at the time of cataract surgery (ironically, being young increases risk)
- Certain surgical techniques
- Inflammation after surgery
- Pre-existing eye conditions
Because I had cataract surgery at 16, my age alone placed me at a higher risk later on.
Treatment for Secondary Cataracts
The good news? Treatment is straightforward and highly effective.
The procedure is called:
YAG Laser Capsulotomy
This is a quick, painless laser procedure that:
- Takes only a few minutes
- Is done in a clinic setting
- Requires no surgical incision
- Uses a laser to create a small opening in the cloudy capsule
- Immediately restores clear vision in most cases
Light can once again pass cleanly through to the retina; unlike the original cataract surgery, this treatment is typically much simpler, and recovery is fast.
Conclusion
I’m waiting for the prognosis on my eyesight and the secondary cataract, and I can’t help feeling a bit anxious about the wobbly lens in my right eye, the one I had implanted when I was 16. I know secondary cataracts are common after surgery and usually treated with a straightforward YAG laser procedure, but the uncertainty still weighs on me. Even so, I’m holding onto the hope that with the pace of modern technology, my vision might one day be fully restored. I’m especially encouraged by the progress in advanced intraocular lenses and early bionic‑eye research. At the moment, fully implantable bionic eye systems and “bionic lenses”, the interventions are only available in the USA, and are still in development or limited to clinical trials. Current reporting suggests that proposed “bionic lens” procedures, such as the Ocumetics Bionic Lens, have been estimated at around $16,000 – $20,000 per eye, though these technologies are not yet commercially available or clinically approved in the UK.
Further Reading & Resources
- Posterior Capsular Opacification (PCO) and YAG Laser Capsulotomy :: Kingston and Richmond NHS Foundation Trust
- Secondary Cataracts: Causes, Symptoms, and Treatment | MyVision.org
- Intraocular Lens (IOL) Implants: Purpose, Procedure, Risks, & Recovery
- IOL Implants: Lens Replacement After Cataracts – American Academy of Ophthalmology
- IOLs (Intraocular Lens): Pros and Cons
- Cataract surgery lens replacement options – Moorfields Private
- Selecting an IOL and Fixation Technique for Patients With UGH Syndrome – Glaucoma Today
- Correct-IOL-implantation-in-cataract-surgery-quality-standard-1.pdf
- Posterior Capsular Opacification: Symptoms, Causes & Treatment
- 20 Questions Patients Commonly Ask About Secondary Cataracts
- Secondary Cataract: Causes, Symptoms, and Treatment
- https://disabledentrepreneur.uk/category/vision-problems/
- https://disabledentrepreneur.uk/category/visual-impairment/
- https://disabledentrepreneur.uk/category/cataract-surgery/
- BIONIC EYES & LENSES
- Can bionic eyes restore vision? Breakthroughs, challenges, and future frontiers in ophthalmology – A comprehensive review – PMC
- Bionic Lens: You’ve never seen anything like it!
- Home – Ocumetics Technology Corp
- Bionic Eyes: Visual Prostheses & Eye Implants
- Bionic Eyes for the Blind: What to Know
- Electromechanical Intraocular Lenses: The Next Step Toward Bionic Vision – London Cataract Centre
- Ocumetics Bionic Eye Lens Updates | DW
- Guide to Bionic Eyes: Implants, Lenses & the Status in 2022 – NVISION
- The Bionic Lens Could Push Eyesight Beyond 20/20 Vision
- Bionic Eyes: Everything You Need to Know | MyVision.org
- Bionic Eye. (December 2022). Britannica.
- Bionic Eyes: Obsolete Tech Leaves Patients in the Dark. (February 2022). BBC.
- Bionic Eyes: Treatments for Blindness Target the Retina and the Brain. (May 2022). Drug Discovery News.
- FDA Approves First Bionic Eye for the Blind. (February 2013). Argonne National Laboratory.
- Medicare Approves Coverage for Second Sight’s Argus II ‘Bionic Eye’. (August 2013). Mass Device.
- Building the Bionic Eye: An Emerging Reality and Opportunity. (April 2016). Progress in Brain Research.
- Advances in Implantable Bionic Devices for Blindness: A Review. (September 2016). Anz Journal of Surgery.

Zena graduated with a Distinction in MSc International Business Management | First Class Graduate in BA (Hons) Marketing Management | Distinction in CIM Level 4 Digital Marketing Techniques
Zena is the co-founder and sub-editor of DisabledEntrepreneur.UK & DisbilityUK.co.uk Zena may look normal to an untrained eye even though she has an invisible disability, thanks to a great support network she is able to adapt into society and has additional help, whenever she needs it.
Zena aspires to be a role model for young people with Multiple Sclerosis. She too suffers from MS and encounters chronic pain symptoms in the legs and has noticed cognitive impairment and muscle weakness.
Recognized as a 'Cosmetic Champion Influencer', she celebrates the innovation, glamour, and empowering spirit that define Disabled Entrepreneur - Disability UK Affiliate Partner Beauty Ranges.
When it comes to marketing Zena works remotely which does not put an added strain on her health. She writes articles and posts on an array of subjects, namely health and wellbeing, business,. She also does social media management, content creation and digital marketing, whilst promoting DisabledEntrepreneur.uk and DisabilityUK.co.uk brands.







